For years, chronic pain and mental health have been treated as separate islands—patients are often forced to drive to one clinic for back pain and a completely different office for depression. But science and experience tell us this fragmented approach fails because:
Chronic pain and mental health are physically interconnected in the brain.
At Pacific Pain & Wellness Group in Torrance, CA, we treat the whole person. Led by Dr. Kartik Ananth—who holds dual board certifications in both Pain Management and Psychiatry—our team is uniquely qualified to bridge the gap between physical relief and emotional stability.
Why Mental Health and Chronic Pain Are Linked
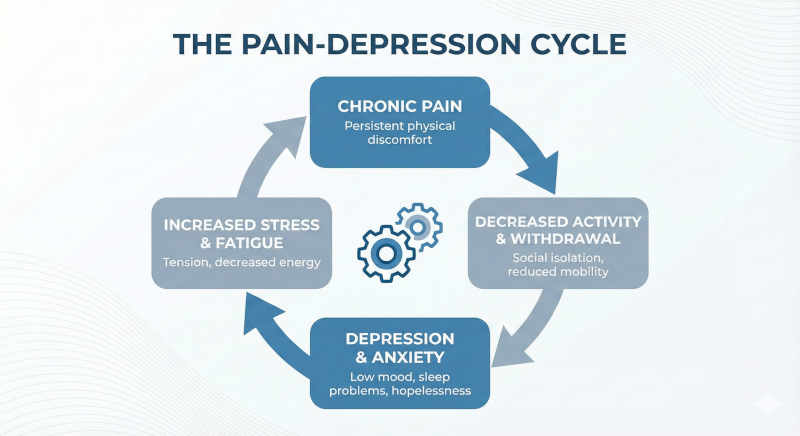
Chronic pain is never "just physical." It hijacks the nervous system, affecting mood, energy, concentration, and sleep. Conversely, untreated anxiety and trauma can physically amplify pain signals, creating a debilitating loop.
The Neuroscience: Shared Pathways
Research confirms that the same regions of the brain that regulate mood also process pain signals. When your mood is dysregulated—due to stress, depression, or anxiety—your body’s natural threshold for pain drops. This is why integrating psychiatric care into pain management is not just "nice to have"—it is essential for long-term recovery.
1. Depression Amplifies Pain
Up to 50% of individuals in the Los Angeles area living with chronic pain also struggle with depression. The loss of mobility and independence creates a cycle where pain worsens depression, and depression chemically makes pain hurt more. Treating only the back or neck without treating the brain leads to incomplete relief.
2. Anxiety Tightens the Body
Anxiety puts the body in "fight or flight" mode, increasing muscle tension and inflammation. Many chronic pain patients experience panic symptoms during flare-ups because the nervous system is stuck in a stress response.
3. Trauma and the Nervous System
For individuals with past trauma, the nervous system often remains on high alert (hyperarousal). This contributes heavily to conditions like fibromyalgia and tension headaches. Our trauma-informed therapy helps reset these alarm systems.
4. Stress Fuels Inflammation
Chronic stress spikes cortisol, which increases inflammation throughout the body. Addressing stress is a medical necessity for effective pain management.
The Problem with Treating Them Separately
When you treat pain without addressing the mind, results are often temporary.
- Scenario A: You receive an injection that relieves back pain, but untreated stress and insomnia cause the muscles to seize up again within weeks.
- Scenario B: You take antidepressants, but unmanaged physical pain keeps you bedridden, preventing the behavioral activation needed to improve your mood.
This is why Pacific Pain & Wellness Group uses an integrated psychiatry + pain management model. We don't just refer you out; we handle both aspects in-house at our South Bay clinic.
Our Whole-Person Model: How We Do It at Pacific Pain & Wellness Group
Because of our dual expertise, we can create a synchronized treatment plan. Here is how our comprehensive approach works:
Step 1: The Dual Evaluation
We don't look at just your MRI, and we don't look at just your symptom checklist. We evaluate:
- Physical pain history and injury mechanics
- Emotional health and neurochemistry
- Sleep architecture (how well you rest)
- Current medications (optimizing for both pain and mood)
- Life stressors impacting your recovery
Step 2: The Integrated Treatment Plan
We combine modalities that amplify each other:
1. Psychiatry & Medication Management
Our psychiatric providers help stabilize neurochemistry. By treating the depression or anxiety, we often see patient pain scores drop significantly. Learn more: Psychiatry & Medication Management.
2. Therapy & Counseling
We use tools like Cognitive Behavioral Therapy (CBT) for Pain and mindfulness strategies to help you unlearn fear-avoidance behaviors and regain control over your life. Explore services: Therapy & Counseling.
3. Interventional Pain Management
Our specialists use targeted interventions—such as epidurals, nerve blocks, or radiofrequency ablation—to "turn down the volume" on pain signals, making it easier for you to engage in therapy and daily life. See our Pain Management Services.
Advanced Care for Complex Cases: TMS & Ketamine
For patients who have tried standard treatments without success, Pacific Pain & Wellness Group offers advanced neuro-therapies.
TMS Therapy (Transcranial Magnetic Stimulation)
TMS is an FDA-cleared, non-invasive treatment for depression. It is ideal for pain patients who may not tolerate additional medications. By reactivating specific areas of the brain, TMS can lift the heavy fog of depression, improving energy and pain tolerance.
Ketamine Infusion Therapy
As pioneers in Ketamine therapy in Los Angeles, we utilize this treatment for severe depression, CRPS, and neuropathic pain. Ketamine infusions work on the NMDA receptors to rapidly reset pain pathways and boost neuroplasticity.
The "South Bay Difference": Why Integration Matters
Patients who utilize our combined approach report:
- Lower pain scores and fewer flare-ups
- Reduced reliance on opioid medications
- Better sleep and higher energy levels
- A return to hobbies and work
You are not just a spine, and you are not just a diagnosis. You are a whole person, and you deserve a doctor who treats you that way.
Stop Choosing Between Mental and Physical Health
If you are in Torrance, Palos Verdes, Redondo Beach, or the greater Los Angeles area, Pacific Pain & Wellness Group is ready to help you find balance.
Schedule your comprehensive evaluation today and experience the difference of dual-board certified care.
